Abstract
Background: Cervical cancer remains a leading cause of cancer-related mortality among women in sub-Saharan Africa. In Gabon, where
screening programs are limited, the introduction of molecular HPV testing could significantly improve early detection.
Objective: To assess the feasibility and epidemiological profile of HPV infection among women screened at the Marcel Abéké Hospital in
Moanda using the Xpert HPV test.
Methods: A cross-sectional pilot study was conducted from March to July 2025 among sexually active women aged 30–65 years. Cervical samples
were collected and analyzed using the GeneXpert platform. Sociodemographic and clinical data were collected via structured questionnaires.
Statistical analyses were performed to identify factors associated with HPV positivity.
Results: Among 206 women tested, the overall HPV prevalence was 18.9%. The most common genotypes were HPV-31/33/35/52/58 (43.9%),
followed by HPV-39/68/56/66 (22.0%). HPV-positive women were significantly younger (mean age 36.3 vs. 40.8 years, p = 0.001) and had
lower gravidity (4.5 vs. 5.6, p = 0.037). No significant associations were found with education level, social status, or screening site.
Conclusion: The Xpert HPV test proved feasible and effective in this setting. Younger age and lower gravidity were associated with HPV positivity.
These findings support the integration of molecular HPV testing into national screening strategies in Gabon.
Keywords: Cervical Cancer; HPV Infection; Cervical Samples
Abbreviations: CCU: Cervical Cancer; HPV: high-Risk Human Papillomavirus; VIA: Visual Inspection with Acetic Acid;
Introduction
Cervical cancer (CCU) is the fourth most common cancer among women globally and the second most prevalent in Gabon, with an incidence of 32.5% and a mortality rate of 17.8% [1]. Despite being preventable through early detection and treatment of precancerous lesions, CCU remains a major public health concern in sub-Saharan Africa due to limited access to screening and treatment services [2]. Persistent infection with high-risk human papillomavirus (HPV) types is the primary cause of CCU [3]. In Gabon, previous studies have reported high HPV prevalence, with oncogenic genotypes such as HPV-16, -18, -33, and -58 being predominant [4,5]. However, most data originate from Libreville, the capital, leaving a knowledge gap in rural and semi-urban regions. To address this, a pilot study was initiated in Moanda, southeastern Gabon, to assess the feasibility of introducing molecular HPV testing using the Xpert HPV assay. This study aimed to evaluate the epidemiological profile of HPV infection and identify associated risk factors among women in this region.
Materials and Methods
Study Design and Setting: this was a prospective, crosssectional, descriptive, and analytical study conducted between March and July 2025. The study was based at the maternity ward and molecular biology unit of the Marcel Abéké Hospital (HMA) in Moanda, with additional recruitment from surrounding health centers in Bakoumba, Mounana, Sucaf and Mvéngué.
Study Population: Eligible participants were sexually active women aged 30 to 65 years, residing in the study area. Women were recruited during routine consultations or through community sensitization campaigns. Informed consent was obtained from all participants.
Inclusion Criteria: Age 30–65 years; Sexually active; Not menstruating at the time of screening; Provided informed consent.
Exclusion Criteria: Never sexually active; Pregnant beyond 10 weeks; Diagnosed uterine pathology; History of cervical cancer; Currently menstruating.
Sample Collection and HPV Testing: Cervical samples were collected using single-use cytobrushes, either by trained healthcare workers or via self-sampling after instruction. Samples were preserved at 4°C and analyzed using the GeneXpert platform (Cepheid), which detects 14 high-risk HPV genotypes, including HPV-16, 18/45, and grouped types such as 31/33/35/52/58.
Data Collection: A structured questionnaire captured sociodemographic data, reproductive history, sexual behavior, and perceptions of HPV screening. Data were anonymized and entered into a secure database.
Follow-Up and Management: HPV-positive women were recalled for visual inspection with acetic acid (VIA) and Lugol’s iodine, followed by colposcopy and biopsy if needed. Women with suspected invasive cancer were referred to the Libreville Cancer Institute for further management.
Statistical Analysis: Descriptive statistics summarized the population characteristics. Student’s t-test and chi-square tests were used to compare variables between HPV-positive and HPVnegative groups. A p-value < 0.05 was considered statistically significant.
Results
Participant Characteristics: Out of 315 eligible women, 206 were tested (100% participation rate). The mean age was 39.9 years, with a mean age at first sexual intercourse of 17.1 years. The average gravidity was 5.4 and parity 3.6. The test invalidity rate was 2.8%, and 93% of women retrieved their results.
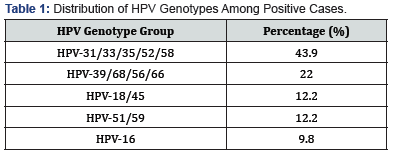
HPV Prevalence and Genotype Distribution: Overall HPV prevalence: 18.9% (39/206). Most frequent genotypes: HPV- 31/33/35/52/58: 43.9%; HPV-39/68/56/66: 22.0%; HPV-18/45 and HPV-51/59: 12.2% each; HPV-16: 9.8% (Table 1).
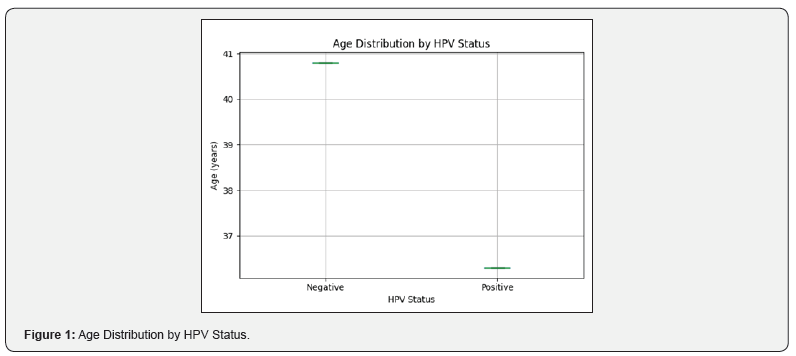
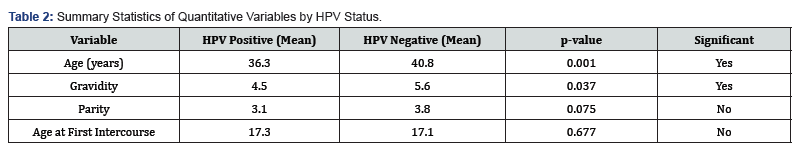
Factors Associated with HPV Positivity: HPV-positive women were significantly younger (mean age 36.3 vs. 40.8 years, p = 0.001) and had lower gravidity (4.5 vs. 5.6, p = 0.037). No statistically significant associations were found with parity, age at first intercourse, education level, social status, or screening site (Table 2 and Figure 1).
Discussion
This study confirms the feasibility of implementing molecular HPV testing in a semi-urban setting in Gabon. The observed HPV prevalence (18.9%) aligns with findings from similar African contexts [6,7]. The predominance of genotypes such as HPV- 31/33/35/52/58 and HPV-39/68/56/66 reflects regional genotype distribution patterns. The significant association between younger age and HPV positivity is consistent with global data showing peak HPV acquisition shortly after sexual debut. Lower gravidity among HPV-positive women may reflect shorter exposure time or differences in immune response. The lack of association with education or social status suggests that HPV infection is widespread across socioeconomic strata in this population. The high rate of result retrieval and questionnaire completeness (95%) indicates strong community engagement and acceptability.
Study Limitations
This study has several limitations that should be considered
when interpreting the findings:
Sample Size and Generalizability: The sample remains
relatively small and geographically limited to Moanda and
surrounding areas, which may affect generalizability.
Cross-Sectional Design: Limits the ability to establish causal
relationships between HPV infection and associated risk factors.
Self-Reported Data: May be subject to recall bias or social
desirability bias.
Limited Genotyping Resolution: Grouped genotypes limit
assessment of individual genotype prevalence.
Lack of Histopathological Confirmation: Not all HPVpositive
women underwent biopsy.
Potential Selection Bias: Participants may differ from women
less engaged with the healthcare system.
Short Follow-Up Period: No long-term follow-up to assess
outcomes of HPV-positive women.
References
- GLOBOCAN Gabon (2022) International Agency for Research on Cancer.
- Sankaranarayanan R, AM Budukh, R Rajkumar (2001) Effective screening programmes for cervical cancer in low- and middle-income countries. Bull WHO 79(10): 954-62.
- Clifford GM, et al. Worldwide distribution of HPV types in cytologically normal women. Lancet 366: 991-998.
- Si-Mohamed A, et al. (2005) High prevalence of high-risk HPV in women in Libreville, Gabon. J Med Virol 77(3): 430-438.
- Zoa-Assoumou S, Ndjoyi-Mbiguino A, Mabika BM, Belembaogo E, Khattabi A, et al. (2016) HPV genotypes in cervical cancer cases in Gabon. Infect Agent Cancer 11:42.
- Denny L, Kuhn L, Hu CC, Tsai WY, Thomas C Wright (2010) HPV-based cervical cancer prevention: long-term results of a randomized screening trial. J Natl Cancer Inst 102(20): 1557-1567.
- Qiao YL, Sellors JW, Eder PS, Bao YP, Lim JM, et al. (2008) A new HPV-DNA test for cervical-cancer screening in developing regions. Lancet Oncol 9(10): 929-936.